A moderate amount of sunlight stimulates the body and mind in many ways. Sunlight in higher dosage causes premature skin aging and still more of it will induce photo- damages. The tightrope walk now consists of benefitting from the positive effects of our health while avoiding premature skin aging and serious damage to our skin.
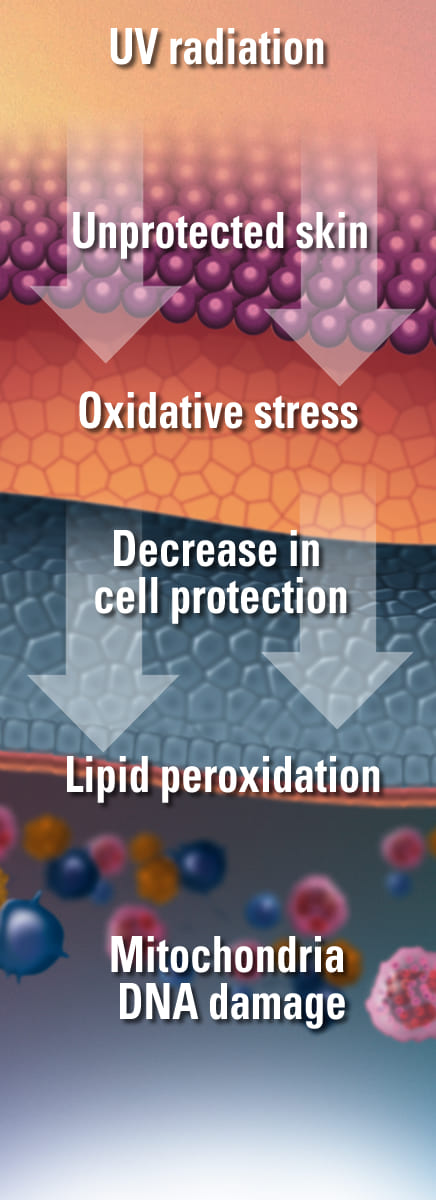 Sun radiation consists of several wavelengths that penetrate varyingly deep into the skin and trigger many different reactions. Almost every wavelength can induce radical formation either with protective, recovering or damaging effects. Thus, radiation and radicals stimulate the melanin formation (skin protection), initiate the vitamin D3 synthesis (health), combined with warmness they have anti-inflammatory effects (healing), strengthen the immune system (prevention against infections), trigger inflammations (sunburn), stimulate collagen-degrading enzymes (aging) or cause DNA modifications (carcinogenesis).
Sun radiation consists of several wavelengths that penetrate varyingly deep into the skin and trigger many different reactions. Almost every wavelength can induce radical formation either with protective, recovering or damaging effects. Thus, radiation and radicals stimulate the melanin formation (skin protection), initiate the vitamin D3 synthesis (health), combined with warmness they have anti-inflammatory effects (healing), strengthen the immune system (prevention against infections), trigger inflammations (sunburn), stimulate collagen-degrading enzymes (aging) or cause DNA modifications (carcinogenesis).
The dose makes the poison
The principle of Paracelsus[1] means that the dosage determines whether a substance is harmful, and this also applies to physical impacts such as radiation and energy. A moderate amount of energy in the form of warmness (low dosage) is beneficial while heat (high dosage) is harmful and can even lead to burns.
With regard to radiation, the severity depends on the acquired self-protection. Sounds like granny’s advice of starting with short sun exposures and gradually prolonging them so that the self-protection can be built up through melanin formation.
Background: melanin transforms almost up to 100% of the UV radiation into heat. However, similar to any other sunscreen it only has a limited effect that depends on the distribution of melanocytes and the melanosomes they provide for the transport into the keratinocytes.
Without external skin protection, the UV-A radiation (315-380 nm) penetrates as deep as the dermis layer (sclera), builds up radicals and damages the collagen structures. The skin aging process is accelerated. The risk of erythema is low, however, due to the DNA-damages there is a serious risk of specific forms of skin cancer.
UV-B radiation (280-315 nm) gets into the epidermis (cuticle) and is responsible for sunburns (erythema) which involve an increased skin cancer risk. UV-B also induces melanin formation and hence prolongs the natural self-protection time. Small amounts of UV-B are beneficial for our health because of the induced Vitamin D3 formation (cholecalciferol). Sunlight also comprises UV-C radiation (100-280 nm) that is already absorbed in the upper atmosphere.
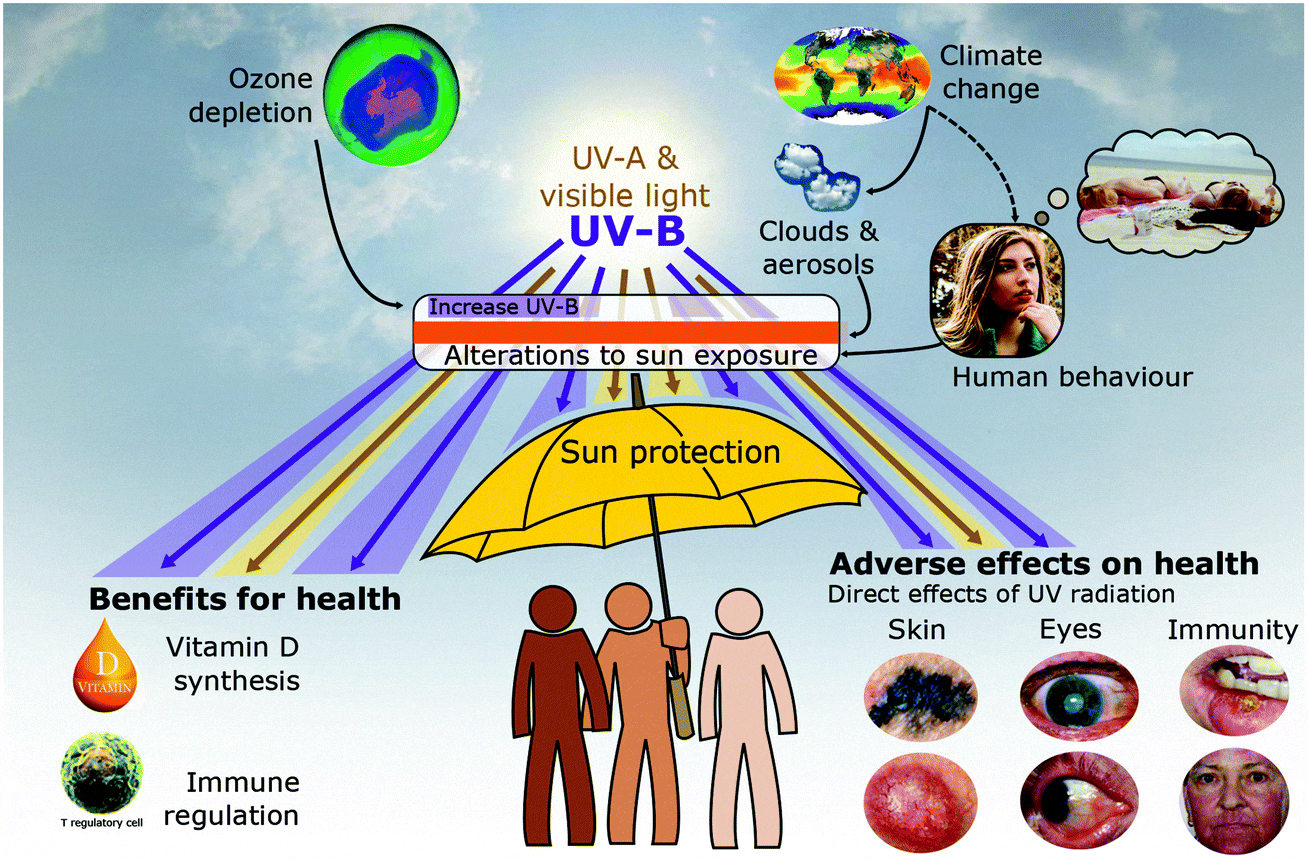
Sun protection factors (SPF)
Considering the UV-B radiation, the sun protection factor (SPF) of a preparation is defined by taking the minimum erythema dose of the protected skin and dividing it by the minimum erythema dose of the unprotected skin.
Results are: self-protection time x SPF = maximum sun exposure.
The EU icon – the letters UVA encircled – means: The UV-A protection amounts to at least one-third of the UV-B filter. Sun protection factors are specified with an amount of 2 mg of sunscreen application per square centimetre of skin. This means that just as much sun screen should be applied onto the skin.
The UV-A protection either is measured in accordance with the in-vivo PPD-method (PPD = Persistent Pigment Darkening) or a correlating in-vitro measuring established by COLIPA (European Cosmetics Association).
The additional information on the critical wave length is a quality feature of the filter and allows a technical statement on the long-wave range of the UV-A filter.
There are different SPF standards depending on the different countries.
Europe: ISO 2444:2010 and ISO 24443:2012 (UV-A).
US: FDA 2011 21 CFR Parts 201/310 (annotation: the licensed filters are obsolete and allow a relatively high radical formation).
Australia/New Zealand: AS/NZS 2604:1998; due to the predominantly Celtic skin an SPF of at least 25 is required by law.
Japan also has its own standard. The values of the different filter standards are not comparable. The efficacy of the European standard SPF 6 complies with 83.3% of sun protection, of 10: 90%; 15: 93.3%; 20: 95%; 25: 96%; 30: 96.7%; 50: 98%; 50+ >98%.
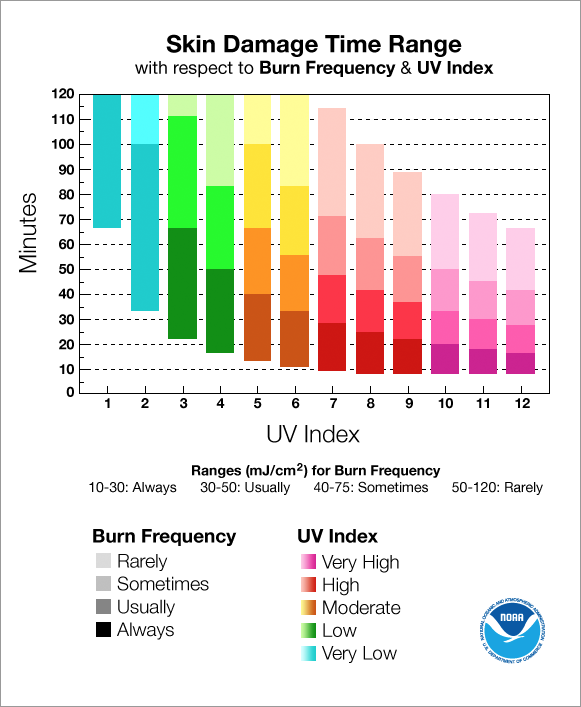
Self-protection time of the skin
In order to make an estimate on the individual maximum sun exposure, it is necessary to know the dependence of self-protection time from local and atmospheric factors. Hence the self-protection time at noon local time naturally is at its minimum (mind daylight saving time!); furthermore there is a minimum on the 21st June on the northern hemisphere and the 21st December in the southern hemisphere. There are two minima at the equator, namely 21st March and 23rd September.
Other factors such as the altitude in the mountains, relatively pure air, and high radiation reflection through water, sand and snow also reduce the self-protection time while it augments with increasing cloudiness. In the case of fog and high fog, the leakage radiation has to be considered, though.
The UV-index (UVI) of the Federal Office for Radiation Protection (Bundesamt für Strahlen- schutz – BfS) offers information on the UV- radiation for various places worldwide. In Germany, it is around 0 in wintertime and summer around 8 at maximum; at the equator and highest position of the sun it is up to 13 (for example Singapore, at sea level). As a rule of thumb, the SPF should be at least 2 x UVI for small children 4 x UVI, and it has to be mentioned that small children should not be exposed to sun radiation without any sun protection. The Celtic skin type is very sensitive with a self-protection time of only 5-10 minutes in Central Europe.
Sun protection products
The sun protection factors of sunscreens have to be individually measured in a way that they render harmless the remaining radiation that is not absorbed by melanin, in other words, transform it into heat. This ensures that both the melanin formation for the protection of the skin and the vitamin D3-synthesis still are stimulated.
Additional antioxidants are counterproductive since they inhibit tyrosinase and melanin formation. That also applies to the preparations administered during the radical-controlled recovery process after the sunburn. Also, their fast degradation due to the impact of radiation and atmospheric oxygen is a relevant argument against the use of antioxidants. They would have to be administered in disproportionally high concentrations, though. High doses of vitamin C and vitamin E however trigger pro-oxidative radical chain reactions.
Sun screen products cannot protect against the intense infrared radiation of the sun that significantly accelerates the premature skin aging process through collagen degradation, among other factors. Infrared radiation in moderate doses however can have regenerative effects (cf. infrared lamp) and thus stimulate healing processes.
Radical scavengers instead of all-day protection
There is little point in using day creams with UV filters for the daily skincare routine. Attention should however be paid to the optimum support of the skin with NMF substances (amino acids) which are natural radical scavengers.
In cases where hyperpigmentation should be prevented, melanin-inhibiting active agents such as ascorbyl phosphate (vitamin C-phosphate), azelaic acid, tranexamic acid, kojic acid, and niacinamide with phosphatidylcholine as a liposomal carrier are recommended besides avoiding exposure to sun radiation.
After-Sun preparations
Topically applied ω-3- and ω-6-fatty acids in the form of nano dispersed aqueous solutions of linseed-, kiwi seed-, evening primrose-, borage-, and rosehip seed oil as well as phosphatidylcholine and echinacea extract (alias coneflower) have anti-inflammatory effects after sunburns. Creams with appropriate active agents can only be applied after the skin surface is dry. In cases where bacterial interactions can be expected, Boswellia extract (protease inhibitor), azelaic acid (5-α-reductase inhibitor), and phosphatidylserine (activation of macrophages) are adequate additives.
Appropriate regenerative active agents for after-sun preparations are retinoids – such as vitamin A (retinol) and its ester, retinal (aldehyde), provitamin A (carotenoids; astaxanthin)
– and vitamin B3 (niacinamide) as well as pro- vitamin B5 (D-panthenol).
Besides sunburns also photodamages in the form of photosensitization and irritations can appear. They can be triggered by medical drugs, as e.g. psychotropic drugs, cytostatics, chemotherapeutic substances and St. John’s wort preparations (alias Hypericum perforatum; over-the-counter drug) as well as cosmetic ingredients such as terpenes (e.g. ascaridol formation from tea tree oil), bergamot oil (bergapten), polyethylene glycols (peroxides) and unsaturated oils (peroxides); but also contacts with cartwheel flower (alias giant hogweed, giant cow parsley) and cow parsnip (alias eltrot, hogweed) (furocoumarins) in combination with sun exposure have to be mentioned in this context. As far as hyperpigmentations are concerned they can be gradually removed with pharmaceutical and cosmetic acid peelings as well as microdermabrasion.
Inflammatory processes require medical attendance.
In this context post-inflammatory or frequency- related hyperpigmentations should be mentioned which can be inhibited by administering liposomal ascorbyl phosphate before and after the laser treatments.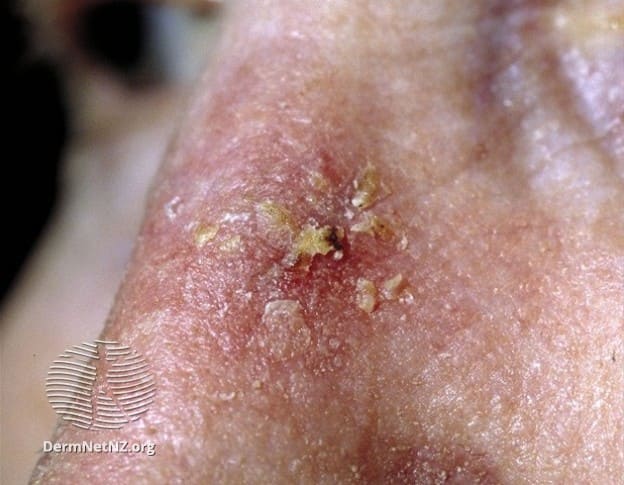 Actinic keratosis can be a consequence of repeated or prolonged sun exposure. The dermatological treatment comprises, among others, diclofenac, 5-fluorouracil or photodynamic therapy (5-aminolevulinic acid/ cold red light), while the cosmetic indication-accompa- nying treatment is Boswellia extract.
Actinic keratosis can be a consequence of repeated or prolonged sun exposure. The dermatological treatment comprises, among others, diclofenac, 5-fluorouracil or photodynamic therapy (5-aminolevulinic acid/ cold red light), while the cosmetic indication-accompa- nying treatment is Boswellia extract.
Examples of endogenously caused photodermatoses are xeroderma pigmentosum (life-threatening genetic defect – "children of the night"), lupus erythematosus (autoimmune disease), metabolic disorders (e.g. erythropoietic protoporphyria) polymorphous photodermatoses and solar urticaria.
Besides preventive sun screen preparations and abstinence from sun exposure, the skincare focuses on the symptoms and consists of anti-inflammatory substances (see above), anti-itching substances such as urea, astringent preparations (tannic acid, witch hazel) as well as active agents against hyperpigmentations and recovery-supporting agents (see above).
Skincare after γ-radiation treatments
If the skin is the so-called transit organ for medical γ-radiation, adverse effects such as dehydrated skin – together with a high transepidermal water loss (TEWL) can appear. Also redness (erythema and inflammation) can occur similar to a sunburn (radiodermatitis), and matrix-metalloproteinases can be stimulated, which have collagen-degrading effects. The stimulation of tyrosinase (post-inflammatory hyperpigmentation) leads to dark colourations on the skin. Actinic keratosis also can occur.
Indications-accompanying cosmetic skincare focuses on treatments with emulsifier-free and preferably lamellar creams or oleogels (non-aqueous and mineral oil-free). Recommended active agents are moisturizers such as amino acids, alginic acid, CM-glucan, hyaluronic acid, D-panthenol and aloe vera, astringent substances such as witch hazel and green tea, anti-inflammatory components such as essential fatty acids in the form of kiwi seed-, linseed-, evening primrose oil and phosphatidylcholine as well as boswellic acids. The latter-mentioned are protease inhibitors and together with ascorbyl phosphate they also inhibit the collagen degradation. Urea and long-chained carboxylic acid amides impede the itching. With regard to hyperpigmentation and recovery, the above-mentioned ingredients can be administered.
Reference: [1] The principle of Paracelsus
About the author Dr Hans Lautenschläger, PhD
Dr Hans Lautenschläger, PhD
Organic chemist, Managing director of KOKO Kosmetikvertrieb GmbH & Co. KG, Leichlingen, Germany
Fields of activity:
• Development of cosmetic & dermatological products
• Skin protection
• Phospholipids
• Carriers of cosmetic active agents
This article was previously published in Beauty Forum 2020 (3), 68-72 as Quantum of sun- prevention & recovery of photodamaged skin












