By Pia Kynoch
Naturopath, Skin Therapist, Educator
Life on Earth has forever followed the rhythm of the 24-hour solar day, an orchestrated dance governed by circadian rhythms — intricate biological symphonies harmonising internal processes with the predictable cadence of light and darkness. [1]
The term 'circadian' is a fusion of 'circa' (about) and 'dies' (day), in acknowledgment of how light precisely calibrates essential physiological and behavioural events, and this choreography, sculpted through evolutionary adaptation, ensures an optimal internal resonance with the external world. [1]
Our physiological circadian patterns, characterised by 24-hour rhythms, are orchestrated by a biological "master clock" nestled within the suprachiasmatic nuclei (SCN) of the hypothalamus in the brain. [2]
This central clock is finely regulated, and continuous adjustments are necessary to synchronise with the external environment, a process known as entrainment,
utilising external time cues or "zeitgebers". [3]
The principal zeitgeber is the changing light conditions during dawn and dusk,which directly affects the SCN, and non-photic zeitgebers are food, temperature,social engagement and sleep. [2]
Achieving synchronisation via photic and non-photic cues between the central and peripheral body clocks is pivotal for maintaining optimal metabolic function. [39]
The daily light-dark cycle dependent biological clock is a central regulator of physiological functions in nearly all cells, tissues and organs. It governs various intracellular signalling pathways, encompassing activities like cell proliferation,DNA damage repair and response, angiogenesis, heart rate, glymphatic and lymphatic fluid flow, endocrine secretion, liver and kidney function, cutaneous and adipose tissue physiology, metabolic regulation, redox balance, cognitive
performance, inflammatory, as well as adaptive and innate immune responses. [4] ; [39]
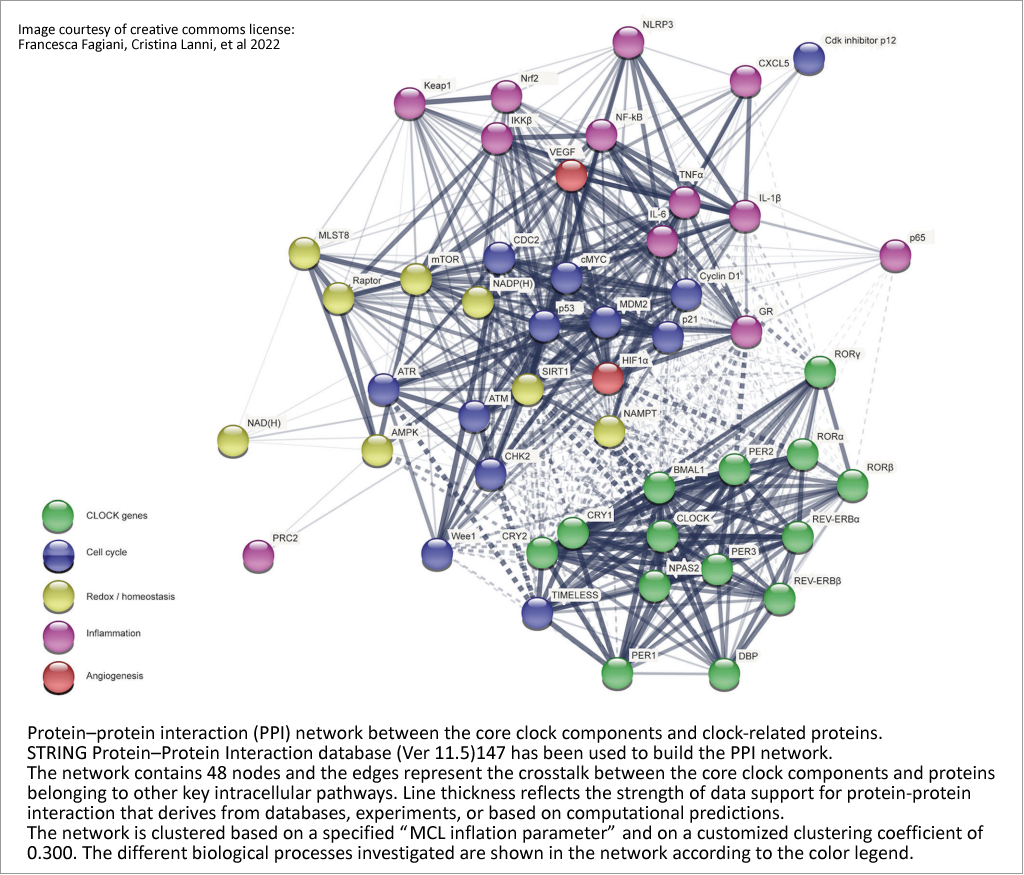
Peripheral body clocks are a part of the circadian rhythm system that exists outside of the central nervous system (Finger and Kramer 2021). These peripheral clocks are present in every organs and tissue throughout the body and are responsible for regulating local physiological processes in response to the external environment, synchronised by the integration of multiple signals. [40] The master clock in the central nervous system is connected to the peripheral organs via the sympathetic branch of the autonomic nervous system. [5]
Circadian rhythms are inherently responsive to light/dark cues, making them susceptible to disruptions from artificial light sources and light pollution in urban areas, particularly at night. [40]; [6] Interestingly, this disruption level appears to vary with sex and age, and with artificial light at night now impacting at least 80% of the world’s population this is now considered a risk factor for the development of diseases across all populations. [40]; [6]
The proliferation of artificial lighting has vastly extended our access and desire for nocturnal activities, allowing individuals to either consciously or unconsciously manipulate their light–dark cycles, creating misalignment with their internal circadian physiology to varying degrees and intensities. [40]; [6]
The absence of circadian system entrainment results in the loss of our body’s ability for "fine-tuning," causing physiological and psychological behaviours to spiral into chaos, a condition termed "internal desynchrony." Despite the paramount importance of entrainment, the mechanisms driving these pathways remain incompletely elucidated and the natural gift of light completely underappreciated in a health care plan. [3]
Circadian misalignment creates, and exacerbates, disease. [39]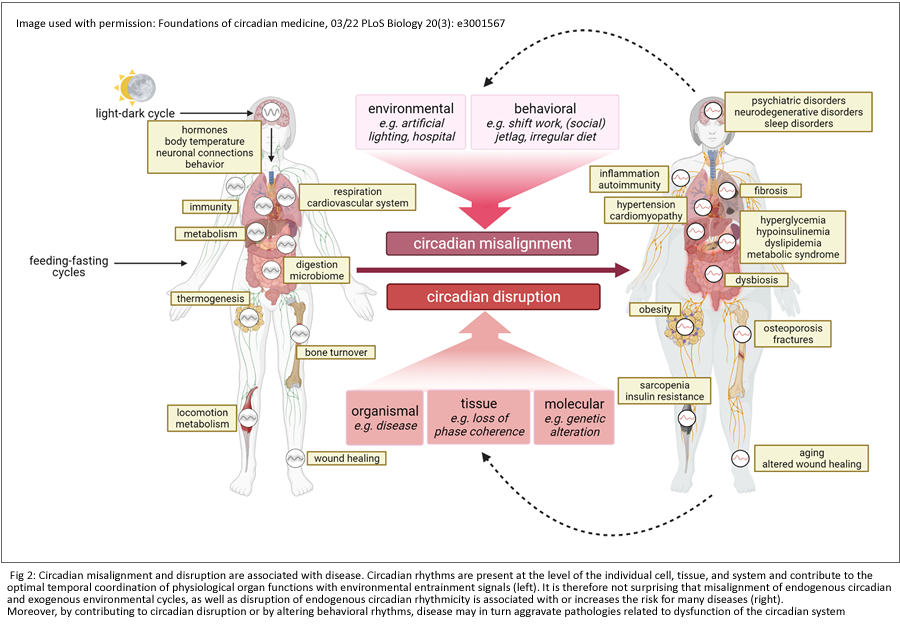
For those skin therapists deeply entrenched in the science of corneotherapy,understanding the impact of circadian biology holds a powerful key to optimising skin health for their clients. The skin, a complex organ that is the focal point of corneotherapeutic interventions, undergoes numerous physiological and biochemical processes influenced by the circadian rhythm. [7]
Skin Health and Circadian Rhythm:
Processes such as cell proliferation, DNA repair, barrier function, and sebum production, all fundamental to corneotherapy, are strongly influenced by the circadian rhythm. [41]
A remarkable function of the skin is its highly complex endocrine system. The presence of equivalents to the HPA and HPT axes, catecholaminergic, cholinergic, steroidogenic, melatoninergic, and secosteroidogenic systems has been extensively described. [8]
There is now compelling evidence that disturbance of circadian coherence can severely undermine these systems, contributing to skin conditions such as acne,eczema, dermatitis, and premature ageing, issues currently managed by corneotherapists that may be missing the pivotal link to circadian biology. [41]
Lipidomic Profile and Circadian Rhythm:
Recent research has shown that the lipidomic profile, the composition and metabolism of lipids in the skin, also follows a circadian rhythm. [9] Lipids play a vital role in maintaining the skin's barrier function, permeability and antimicrobial function, skin hydration, and overall health. [9]
Disruptions in the circadian rhythm can lead to imbalances in the lipidomic profile, contributing to skin conditions like dryness, sensitivity, and inflammation. [9]
The skin communicates with internal organs, and skin lipid metabolism is related to whole-body glucose and lipid metabolism. [10]
Understanding the relationship between the circadian rhythm and the lipidomic profile can help researchers and dermal therapists develop targeted interventions to support optimal skin health and function.
Hormonal Health and Circadian Rhythm:
Hormones like cortisol, often termed the "stress hormone," melatonin, crucial for sleep regulation, and pregnenolone,a precursor to both cortisol and melatonin that can help regulate the balance between the two hormones, are intricately tied to the circadian rhythm. [11]; [12]
Melatonin and cortisol have an inverse relationship, where when one is higher, the other should be lower, and vice versa. [12] Cortisol is a key player in the circadian system that affects nearly every tissue and organ of the body, including the skin, and when dysregulated create a myriad of acute and chronic issues in our tissues. [13]
The balance between melatonin and cortisol is essential for optimal health, and an imbalance between the two can lead to chronic inflammation, recurring infections, mental health issues, brain fog, adrenal exhaustion, chronic illness, and a sharp decline in the quality of life. [14]
Disruptions due to exposure to artificial light at night can disrupt the hormonal balance, a core concern for corneotherapists in their treatment strategies.
Blood Glucose Levels and Circadian Rhythm:
Blood glucose levels play a crucial role in maintaining overall health, including skin health. [15] The regulation of blood glucose levels is influenced by the circadian rhythm, and disruptions in this rhythm can impact glucose regulation, leading to various health issues, including skin problems. [16]; [17]
The circadian system is involved in regulating the daily rhythm of glucose metabolism. [18] Research has shown that there is a direct link between glucocorticoid hormones, which are involved in blood sugar control, and genes that regulate the biological clock. [18]
When blood glucose levels are not properly regulated, it can lead to an increase in advanced glycation end products (AGEs), which can cause damage to collagen and elastin in the skin, leading to premature ageing and the development of wrinkles. [18]; [19]; [20]
2022). Additionally, high blood glucose levels can contribute to inflammation in the body, which can exacerbate skin conditions such as acne, psoriasis,dermatitis and eczema. [20]
Nervous System Regulation and Circadian Rhythm:
The nervous system plays a crucial role in regulating the circadian rhythm and skin health. [21]; [5]
Recent research has shown that disruptions in the circadian rhythm can lead to imbalances in the nervous system, and vice versa, which can impact skin health and contribute to various skin conditions due to changes in immune response, inflammation, skin barrier function, lipid production and sweat response.
The Bidirectional Relationship between Mood Disorders and Circadian Rhythms:
The relationship between skin, which is a highly innervated organ, and mood disorders is complex and multifaceted, with circadian rhythms playing a crucial role in this interaction. [41]; [22]; [23] Disruptions in circadian rhythm have been associated with various mental health conditions, including mood disorders like depression and anxiety. [24]
Skin conditions can cause depression and anxiety: People with common skin disorders such as eczema, psoriasis, rosacea, acne, alopecia, and HSV can experience depression and anxiety due to the demands, intrusions,dysesthesias, and visible signs of these conditions. [25]; [39]
These disruptions can manifest as changes in sleep patterns, hormone rhythms, body temperature rhythms, disruptions to skin healing and exacerbation of skin disease, all of which can impact mood and overall well-being in a viscous loop. [25]; [39]; [8] A population-based study found that participants with skin diseases were more likely to have depressive symptoms, social isolation, loneliness, suicidal thoughts and lower quality of life. [26] The severity of a person's anxiety and/or depression may also correlate with the degree of misalignment in their circadian rhythm. [27]
Microbiome Balance and Immune Modulation:
Corneotherapists, while addressing skin issues, consider the skin microbiome and immune system. Recent research has shown that disruptions in the circadian rhythm can lead to imbalances in the microbiome populations in different compartments on and in the body,, contributing to various skin conditions, including acne, eczema, dermatitis and psoriasis. [28] The gut microbiota and thus gut-skin axis has also been linked to the circadian-metabolic axis, with evidence suggesting that the gut microbiota can modulate host circadian rhythms and metabolic health and vice versa. [28; [29]
Understanding the complex relationship between circadian rhythms, disruptions of the microbiome balance, and immune modulation can help researchers and dermal therapists develop innovative strategies to promote overall well-being and support the skin's natural regenerative processes.
The Impact of Artificial Light on Circadian Biology and Skin Health:
Artificial light exposure can have a significant impact on circadian biology and skin health. Exposure to artificial light, especially at night, can disrupt the circadian rhythm, leading to imbalances in the body's natural processes, including glucose metabolism, hormonal balance, and immune function. [30]
This disruption can also impact skin health, leading to various skin conditions like acne, eczema, dermatitis, and premature ageing. [31]; [6]; [7]
To mitigate the negative effects of artificial light on circadian biology and skin health, it is essential to take measures to limit exposure to artificial light at night and access natural light during the day. [32]; [33]
Here are some strategies to consider:
● Limit screen time before bed: Avoid using electronic devices, such as smartphones and tablets, for at least one hour before bedtime to allow your body to naturally wind down and prepare for sleep.
● Use blue light filters: Install blue light filters on your electronic devices or use blue light-blocking glasses to reduce the impact of blue light on your circadian rhythm and skin health.
● Create a sleep-friendly environment: Make your bedroom a dark,quiet,cool and comfortable space that promotes relaxation and optimal sleep quality. Use blackout curtains or an eye mask to block out any sources of artificial light.
● Prioritise natural light exposure: During the day, spend time outdoors or near open windows to expose yourself to natural light, which can help regulate your circadian rhythm and support optimal skin health. Natural light is made up of different wavelengths, including blue, red, and infrared light, which can have different positive effects on the body and skin health
● Access dawn and dusk: Accessing natural light at dawn and dusk can help regulate the circadian rhythm, improve pregnenolone production and support optimal skin health.
● Utilise indoor highly efficient violet LEDs (blue light free)
● Regular natural skin contact with earth
● Increasing awareness of true physical needs
Earthing, also known as grounding, is the practice of connecting the human body to the Earth's surface electrons. [34] Scientific studies have found that earthing can have significant benefits for human health, including reducing inflammation and pain, improving glucose regulation, enhancing immune response, improving heart rate variability, reducing tension and overall stress levels, and improving healthy sleep, all very relevant to this topic. [35]; [36]
The influx of free electrons absorbed into the body through direct contact with the Earth neutralises free radicals and thereby reduces acute and chronic inflammation and slows ageing (Menigoz et al. 2020). Earthing also reduces electric fields imposed on the body, which can contribute to chronic inflammation. [36]
The anti-inflammatory effects of earthing are due to the negatively charged antioxidant electrons from the Earth entering the body and neutralising the build up of positively charged free radicals. [36]
Earthing has been shown to reduce inflammation as a result of earthing with infrared medical imaging and with measurements of blood chemistry and white blood cell counts. [37
The Earth's surface is an abundant source of excited and mobile electrons, which can rapidly resolve inflammation - and if accessed at dawn and dusk even more benefits may be available as the circadian clocks synchronise. [37]; [38]
In the modern era, artificial light significantly impacts circadian biology and,consequently, skin health. [6]
Corneotherapists need to educate their clients about mitigating these effects for optimal outcomes post-treatment. Taking measures to optimise circadian rhythms, limit exposure to artificial light at night, access natural light during the day and earthing can help mitigate the negative effects of artificial light on the body's natural processes and promote optimal skin health.
About the Author; Pia Kynoch
As an industry educator, speaker, and author, Pia is passionate about catalysing a paradigm shift towards a root-cause approach for healing and transformation. Her journey in education and holistic wellness has been shaped by an array of formal studies, including Beauty Therapy, Naturopathy, Corneotherapy, Functional Nutrition, NLP, Lymphatic Massage, Feminine Embodiment Yoga, Qi Gong, Reiki, Mindfulness, Breathwork, Quantum Healing, Acupressure, and much more, completed over nearly three decades in the skin, beauty, health and wellness industries.
References used in this article:
[1] El-Esawi, Mohamed A. 2018. Circadian Rhythm: Cellular and Molecular Mechanisms. BoD – Books on Demand.
[2] Fishbein, Anna B., Kristen L. Knutson, and Phyllis C. Zee. 2021. “Circadian Disruption and Human Health.” The Journal of Clinical Investigation 131 (19). https://doi.org/10.1172/JCI148286.
[3] Ashton, Anna, Russell G. Foster, and Aarti Jagannath. 2022. “Photic Entrainment of the Circadian System.” International Journal of Molecular Sciences 23 (2). https://doi.org/10.3390/ijms23020729.
[4] Fagiani, Francesca, Daniele Di Marino, Alice Romagnoli, Cristina Travelli, Davide Voltan, Lorenzo Di Cesare Mannelli, Marco Racchi, Stefano Govoni, and Cristina Lanni. 2022. “Molecular Regulations of Circadian Rhythm and Implications for Physiology and Diseases.” Signal Transduction and Targeted Therapy 7 (1): 41.
[5] García-García, Andrés, and Simón Méndez-Ferrer. 2020. “The Autonomic Nervous System Pulls the Strings to Coordinate Circadian HSC Functions.” Frontiers in Immunology 11 (May): 956.
[6] Zeman, Michal, Monika Okuliarova, and Valentina Sophia Rumanova. 2023. “Disturbances of Hormonal Circadian Rhythms by Light Pollution.” International Journal of Molecular Sciences 24 (8). https://doi.org/10.3390/ijms24087255.
[7] Salazar, Andrew, and Jörg von Hagen. 2023. “Circadian Oscillations in Skin and Their Interconnection with the Cycle of Life.” International Journal of Molecular Sciences 24 (6). https://doi.org/10.3390/ijms24065635.
[8] Jin, Rong, Lan Luo, and Jie Zheng. 2022. “The Trinity of Skin: Skin Homeostasis as a Neuro-Endocrine-Immune Organ.” Life 12 (5).https://doi.org/10.3390/life12050725.
[9] Jia, Yan, Mingyue Zhou, Hong Huang, Yao Gan, Manli Yang, and Ruiheng Ding. 2019. “Characterization of Circadian Human Facial Surface Lipid Composition.” Experimental Dermatology 28 (7): 858–62.
[10] Petrenko, Volodymyr, Flore Sinturel, Ursula Loizides-Mangold, Jonathan Paz Montoya, Simona Chera, Howard Riezman, and Charna Dibner. 2022. “Type 2 Diabetes Disrupts Circadian Orchestration of Lipid Metabolism and Membrane Fluidity in Human Pancreatic Islets.” PLoS Biology 20 (8): e3001725.
[11] Witzig, Melissa, Amandine Grimm, Karen Schmitt, Imane Lejri, Stephan Frank,Steven A. Brown, and Anne Eckert. 2020. “Clock-Controlled Mitochondrial Dynamics Correlates with Cyclic Pregnenolone Synthesis.” Cells 9 (10). https://doi.org/10.3390/cells9102323.
[12] Mohd Azmi, Nor Amira Syahira, Norsham Juliana, Sahar Azmani, Nadia Mohd Effendy, Izuddin Fahmy Abu, Nur Islami Mohd Fahmi Teng, and Srijit Das. 2021.“Cortisol on Circadian Rhythm and Its Effect on Cardiovascular System.” International Journal of Environmental Research and Public Health 18 (2). https://doi.org/10.3390/ijerph18020676.
[13] Jones, Carol, and Christopher Gwenin. 2021. “Cortisol Level Dysregulation and Its Prevalence-Is It Nature’s Alarm Clock?” Physiological Reports 8 (24): e14644.
[14] Koop, Sarah, and Henrik Oster. 2022. “Eat, Sleep, Repeat - Endocrine Regulation of Behavioural Circadian Rhythms.” The FEBS Journal 289 (21): 6543–58.
[15] Rahman, Md Saidur, Khandkar Shaharina Hossain, Sharnali Das, Sushmita Kundu,Elikanah Olusayo Adegoke, Md Ataur Rahman, Md Abdul Hannan, Md Jamal Uddin, and Myung-Geol Pang. 2021. “Role of Insulin in Health and Disease: An Update.” International Journal of Molecular Sciences 22 (12). https://doi.org/10.3390/ijms22126403.
[16] Oosterman, Johanneke E., Suzan Wopereis, and Andries Kalsbeek. 2020. “The Circadian Clock, Shift Work, and Tissue-Specific Insulin Resistance.” Endocrinology 161 (12). https://doi.org/10.1210/endocr/bqaa180.
[17] Okoro, Obumneme Emeka, Emanuela Camera, Enrica Flori, and Monica Ottaviani.2023. “Insulin and the Sebaceous Gland Function.” Frontiers in Physiology 14 (September): 1252972.
[18] Shimba, Akihiro, and Koichi Ikuta. 2020. “Glucocorticoids Regulate Circadian Rhythm of Innate and Adaptive Immunity.” Frontiers in Immunology 11 (September): 2143.
[19] Băbţan, Anida M., Aranka Ilea, Bianca A. Boşca, Maria Crişan, Nausica B. Petrescu,Massimo Collino, Rosa M. Sainz, Jared Q. Gerlach, and Radu S. Câmpian. 2019.“Advanced Glycation End Products as Biomarkers in Systemic Diseases: Premises and Perspectives of Salivary Advanced Glycation End Products.” Biomarkers in Medicine 13 (6): 479–95.
[20] Chen, Chun-Yu, Jia-Qi Zhang, Li Li, Miao-Miao Guo, Yi-Fan He, Yin-Mao Dong,Hong Meng, and Fan Yi. 2022. “Advanced Glycation End Products in the Skin:Molecular Mechanisms, Methods of Measurement, and Inhibitory Pathways.” Frontiers of Medicine 9 (May): 837222.
[21] Blake, Kimbria J., Xin Ru Jiang, and Isaac M. Chiu. 2019. “Neuronal Regulation of Immunity in the Skin and Lungs.” Trends in Neurosciences 42 (8): 537–51.
[22] Duan, Grace Y., and Jonathan I. Silverberg. 2023. “Sleep Impairment in Patients with Chronic Inflammatory Skin Diseases: A Review of Mechanisms and Management.” Journal of the American Academy of Dermatology 88 (2):421–27.
[23] Tsujihana, Kojiro, Kosuke Tanegashima, Yasuko Santo, Hiroyuki Yamada, Sota Akazawa, Ryuta Nakao, Keiko Tominaga, et al. 2022. “Circadian Protection against Bacterial Skin Infection by Epidermal CXCL14-Mediated Innate Immunity.” Proceedings of the National Academy of Sciences of the United States of America 119 (25): e2116027119.
[24] Carpenter, Joanne S., Jacob J. Crouse, Elizabeth M. Scott, Sharon L. Naismith, Chloe Wilson, Jan Scott, Kathleen R. Merikangas, and Ian B. Hickie. 2021. “Circadian Depression: A Mood Disorder Phenotype.” Neuroscience and Biobehavioral Reviews 126 (July): 79–101.
[25] Zhang, Xiu-Jie, Ai-Ping Wang, Tie-Ying Shi, Jun Zhang, Hui Xu, Da-Qiu Wang, and Li Feng. 2019. “The Psychosocial Adaptation of Patients with Skin Disease: A Scoping Review.” BMC Public Health 19 (1): 1404.
[26] Yew, Yik Weng, Amanda Hui Yu Kuan, Lixia Ge, Chun Wei Yap, and Bee Hoon Heng. 2020. “Psychosocial Impact of Skin Diseases: A Population-Based Study.” PloS One 15 (12): e0244765.
[27] Codoñer-Franch, Pilar, Marie Gombert, José Martínez-Raga, and María Carmen Cenit. 2023. “Circadian Disruption and Mental Health: The Chronotherapeutic Potential of Microbiome-Based and Dietary Strategies.” International Journal of Molecular Sciences 24 (8). https://doi.org/10.3390/ijms24087579.
[28] Frazier, Katya, and Eugene B. Chang. 2020. “Intersection of the Gut Microbiome and Circadian Rhythms in Metabolism.” Trends in Endocrinology and Metabolism: TEM 31 (1): 25–36.
[29] De Pessemier, Britta, Lynda Grine, Melanie Debaere, Aglaya Maes, Bernhard Paetzold, and Chris Callewaert. 2021. “Gut-Skin Axis: Current Knowledge of the Interrelationship between Microbial Dysbiosis and Skin Conditions.” Microorganisms 9 (2). https://doi.org/10.3390/microorganisms9020353.
[30] Fleury, Giulia, Anayanci Masís-Vargas, and Andries Kalsbeek. 2020. “Metabolic Implications of Exposure to Light at Night: Lessons from Animal and Human Studies.” Obesity 28 Suppl 1 (Suppl 1): S18–28.
[31] Suitthimeathegorn, Orawan, Cheng Yang, Yanyun Ma, and Wei Liu. 2022. “Direct and Indirect Effects of Blue Light Exposure on Skin: A Review of Published Literature.” Skin Pharmacology and Physiology 35 (6): 305–18.
[32] The Lancet Regional Health-Europe. 2023. “Shedding Light on Light Pollution.” The Lancet Regional Health. Europe 31 (August): 100710.
[33] Falchi, Fabio, Pierantonio Cinzano, Christopher D. Elvidge, David M. Keith, and Abraham Haim. 2011. “Limiting the Impact of Light Pollution on Human Health, Environment and Stellar Visibility.” Journal of Environmental Management 92 (10): 2714–22.
[34] Lin, Chien-Hung, Shih-Ting Tseng, Yao-Chung Chuang, Chun-En Kuo, and Nai-Ching Chen. 2022. “Grounding the Body Improves Sleep Quality in Patients with Mild Alzheimer’s Disease: A Pilot Study.” Healthcare (Basel,Switzerland) 10 (3). https://doi.org/10.3390/healthcare10030581.
[35] Menigoz, Wendy, Tracy T. Latz, Robin A. Ely, Cimone Kamei, Gregory Melvin, and Drew Sinatra. 2020. “Integrative and Lifestyle Medicine Strategies Should Include Earthing (grounding): Review of Research Evidence and Clinical
Observations.” Explore 16 (3): 152–60.
[36] Sinatra, Stephen T., Drew S. Sinatra, Stephen W. Sinatra, and Gaetan Chevalier.2023. “Grounding - The Universal Anti-Inflammatory Remedy.” Biomedical Journal 46 (1): 11–16.
[37] Oschman, James L., Gaétan Chevalier, and Richard Brown. 2015. “The Effects of Grounding (earthing) on Inflammation, the Immune Response, Wound Healing, and Prevention and Treatment of Chronic Inflammatory and Autoimmune Diseases.” Journal of Inflammation Research 8 (March): 83–96.
[38] Olde Engberink, Anneke H. O., Job Huisman, Stephan Michel, and Johanna H.Meijer. 2020. “Brief Light Exposure at Dawn and Dusk Can Encode Day-Length in the Neuronal Network of the Mammalian Circadian Pacemaker.” FASEB Journal: Official Publication of the Federation of
American Societies for Experimental Biology 34 (10): 13685–95.
[39] Kramer, Achim, Tanja Lange, Claudia Spies, Anna-Marie Finger, Daniela Berg, and Henrik Oster. 2022. “Foundations of Circadian Medicine.” PLoS Biology 20 (3):e3001567.
[40] Finger, Anna-Marie, and Achim Kramer. 2021. “Peripheral Clocks Tick Independently of Their Master.” Genes & Development 35 (5-6): 304–6.
[41] Kramer, Nicole E., Victoria E. Cosgrove, Kiley Dunlap, Mehala Subramaniapillai,Roger S. McIntyre, and Trisha Suppes. 2019. “A Clinical Model for Identifying an Inflammatory Phenotype in Mood Disorders.” Journal of Psychiatric Research
113 (June): 148–58.
[41] Alexis B Lyons. Circadian Rhythm and the Skin: A Review of the Literature.https://pubmed.ncbi.nlm.nih.gov/31641418/












