By Dr Ghita Lanzendoerfer-Yu
Scientific Communicator, Independent consultant and writer.
Scientific Advisory Board of I.A.C.
Ghita's blog
The market for cosmetic anti-aging products is booming, especially in China and the USA. The German market is relatively modest, with a volume of USD 1.5 billion in 2016 (1).
Despite the pandemic, forecasts point to further growth, because skin aging is the visible component of aging. Therefore, in all market segments, there are numerous cosmetic products designed to prevent or slow down skin aging. Anti-aging also is important in plastic surgery and in nutritional supplements.
Skin aging actually is about more than wrinkles. Here I want to look at the – literally - underlying mechanisms of skin aging: The aging of connective tissue, the appearance of wrinkles and why, some people just look younger.
Classification of skin aging
Skin aging is a multifactorial event and a highly individual process. In dermatology, the aging process is described as "pathological" and "therapies" are prescribed therefore.
Instructions for the classification of wrinkles on the face are common and that is why I start with them (2).
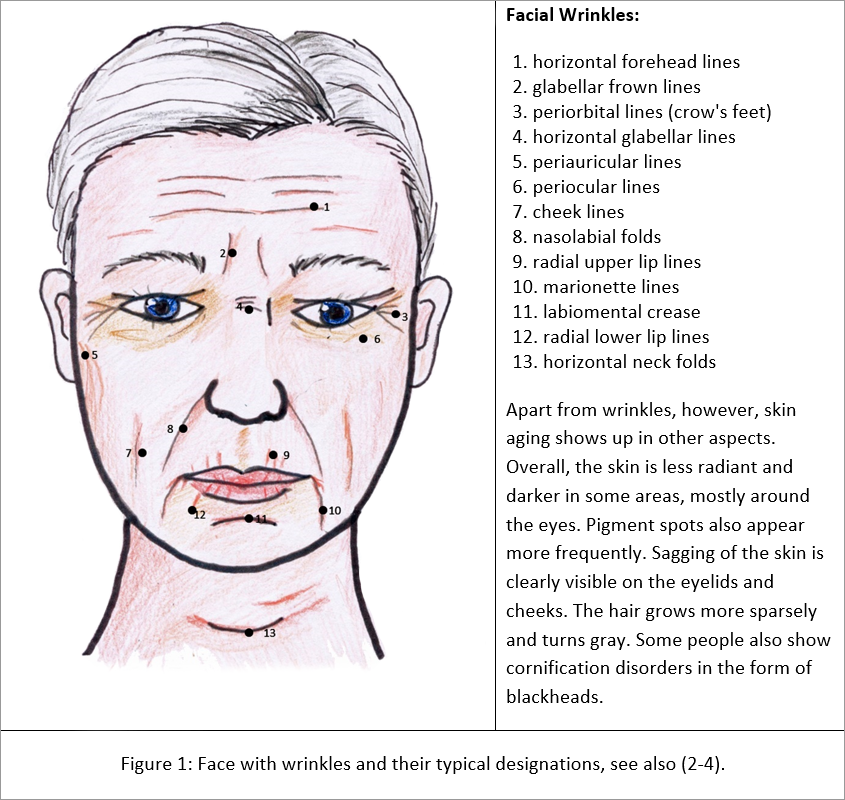
Wrinkles are the most important but by far not the only sign of skin aging. Other parameters are the so-called "sagging" (slackening of the skin), pigment changes and atrophy (tissue loss) (4). In addition, intrinsic and extrinsic factors influence skin aging not only in its development, but also in its course.
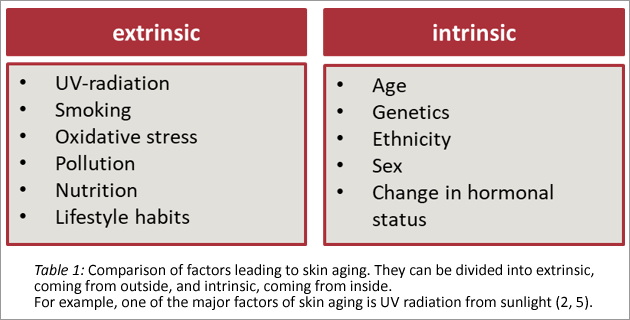
Wrinkles and skin elasticity are measurable parameters (6) that correlate strongly with visually perceived age. Pigment spots as an indication of age are less important in the age assessment of individuals (3).
The relevant aging processes of the skin take place in the dermis, in the extracellular matrix (ECM). And thus, skin aging is definitely not a superficial problem.
The connective tissue of the skin and the Extra Cellular Matrix (ECM)
As the outermost organ of the human body, the skin is built up in several layers. In cosmetics, we deal with the treatment of the epidermis and there specifically with the horny layer (stratum corneum) (9). While the epidermis, like the skin itself, is built up in layers, the underlying dermis is not. It is also often described as connective tissue in general, which is found not only in the skin but in many areas of the body (8-10).
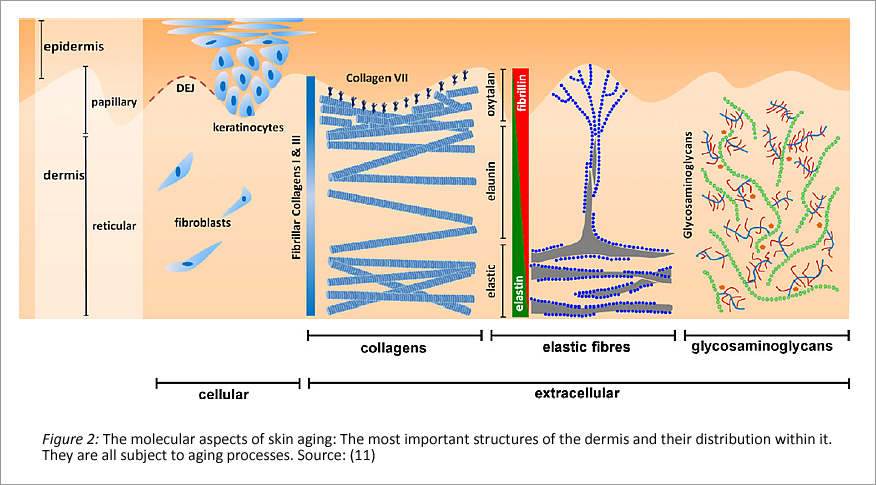
Normally, there are several structures existing in the dermis.
Firstly there are the collagens, which form different networks of varying strength. Embedded in these networks are elastic fibers, elastin, and hygroscopic gels formed from proteoglycans specifically hyaluronic acid. Together they form the extracellular matrix. The cells that secrete these substances are fibroblasts, which are distributed in the collagen network of the dermis.
The connection from epidermis to dermis is established in the basement membrane (dermal epidermal junction, DEJ). Collagen IV is mainly responsible for this.
The role of collagens
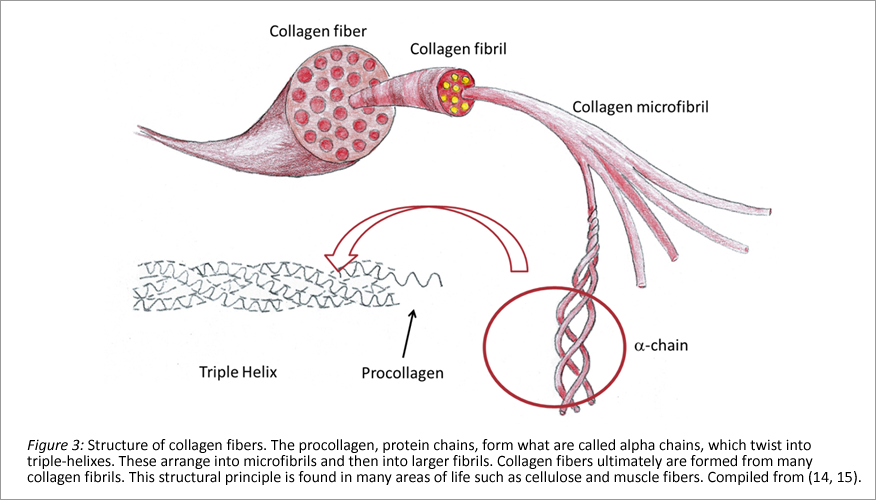
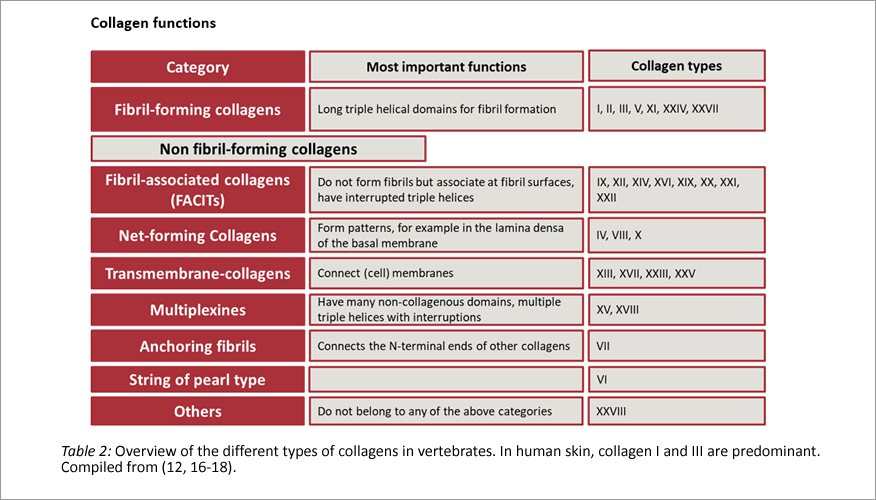
Collagen is the most important structural protein in our body. Collagens are found mainly in connective tissue, but bones, teeth cartilage and skin are also made of collagen. In vertebrates, 28 different types of collagen are known, all with specific properties (12). Responsible for its expression in humans are 43 genes (13).
The biomechanical properties of collagen are caused by the molecular structure of the individual chains, which determine how they twist and what the three-dimensional structure looks like. The essential framework is formed by an amino acid chain, abbreviated GLY-X-Y. GLY is the amino acid glycine, X often is hydroxyproline and Y proline. However, X and Y can also be other amino acids, with which then strands with different mechanical properties are formed.
The elastic properties of the skin - elastin
Elastin is another structural protein of the dermis (19). In addition to the dermis, it is found mainly in the lung and in the vascular walls of the aorta. It contributes resistance and elasticity to the tissue. Elastin is predominantly formed during the fetal and neonatal stages of development. Unlike collagen, it is replenished very little, but has a much longer life span. However, this longer life span and the lack of new formation also mean that wear and tear cannot be eliminated or the molecules are replaced by less elastic substances (20-22).
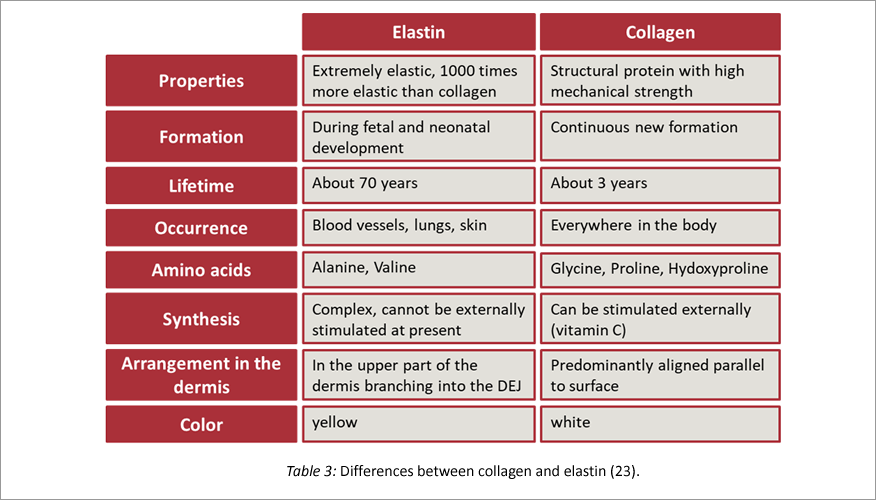
Mechanical stress and wear alter the biomechanical properties of the various skin layers. In particular, the degradation of elastin by proteases reduces the skin's ability to flex.
The skin layers can no longer slide together and must fold (24). Furthermore, the degradation of elastin creates fragments that stimulate inflammation, proliferation or angiogenesis.
Fibroblasts – powerhouse of the ECM
Fibroblasts are the cells of the dermis. Unlike the epidermal keratinocytes, they do not occur in cell aggregates. As synthesis powerhouses, they perform many important functions in the body, most notably wound healing (25, 26) and in inflammatory events of the skin (27).
In the dermis, they produce and organize the ECM. In addition to collagen and elastin, these are proteoglycans and proteases (28, 29).
L'Oréal looked at the role of fibroblasts in skin aging more than 10 years ago. They are also subject to an aging process (30) and alter their turnover.
• Altered morphology and metabolism, decreased proliferative potential
• Loss of sensitivity to growth factors
• Decreased production of ECM components (collagen I and III)
• Overproduction of proteases that degrade them (matrix metalloproteinases MMP)
Proteoglycans - more than a gel cushion
Proteoglycans are the gel formers of the dermis. Here, a protein is coupled to one or more glycosaminoglycans (GAGs). GAGs also occur unbound in the ECM. They are an integral part of the ECM, regulating water content, osmotic balance and fulfilling important immunological functions.
The most important component is hyaluronic acid (31), which plays an essential role in wound healing in the dermis. It is well known as a cosmetic ingredient and has been increasingly used for several years. However, hyaluronic acid of the dermis has a molecular weight of more than 500 Daltons, has anti-inflammatory effects, and promotes the expression of collagen III and growth factors (32). Though, experts contradict the claim that hyaluronic acid could penetrate the skin if it were only low molecular weight (33).
In the course of skin aging, however, proteoglycans are also degraded to smaller fragments and then have a completely different profile of action (34).
Basement membrane - the dermal-epidermal junction
The basement membrane is the layer that connects the basal layer of the epidermis to the dermis. In English it is called "basement membrane" and in technical jargon also "dermal-epidermal-junction" (DEJ). The structural proteins that cause its strength and at the same time allow a certain flexibility have been intensively studied for several years.
This is because the basement membrane plays a major role not only in skin aging, but also in certain diseases such as epidermolysis bullosa (35), or pemphigoid (36) and scarring (37). The epidermal basal layer, which is highly undulated in young skin (and thus has a large surface area) and thus establishes a good connection with the dermis, flattens with age. The interlocking decreases and as a result the quality of the connection. This is due not only to structural changes in this membrane itself, but in the dermis as a whole (38).
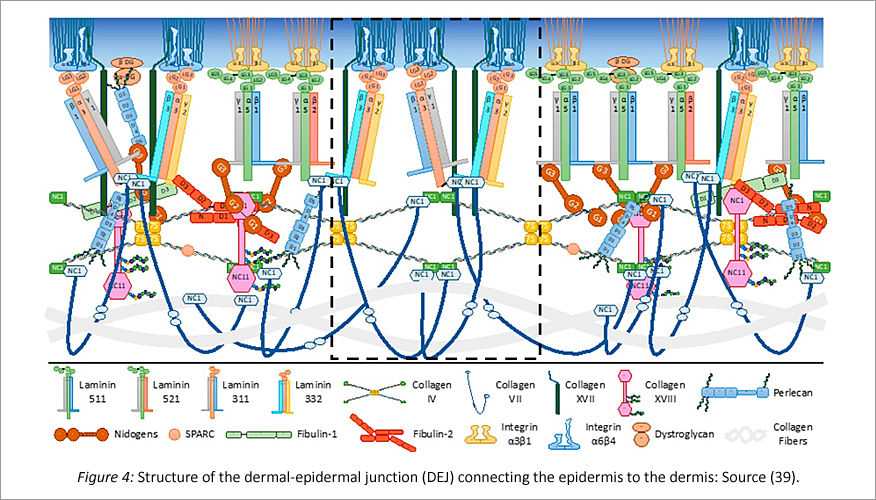
Collagen IV and collagen VII are particularly important for anchoring the epidermis to the dermis. However, besides collagens, many other proteins are involved in the interlocking of the two layers. First of all, there are the laminins, whose research has just begun and of which there are several different types.
Like collagen IV, they can also aggregate themselves (self-assembling) and form elastic networks.
Collagen VII is a typical anchoring protein that connects the collagen I and III fibrils found in the dermis to each other and to the anchor plaques of collagen IV. A network with high mechanical strength is formed. In addition to collagens, laminins, integrins and nidogens are important building blocks in this network.
Collagen IV is found in reduced amounts in aged skin. However, studies on aged fibroblasts in vitro show that collagen IV synthesis can be "boostered" with TGF 1ß in a dose-dependent manner (40).
Skin aging a matter of ethnicity?
Does dark skin age more slowly than light skin (41, 42)? At least some studies might suggest it (43, 44). So it was shown is, that age-related wrinkles appeared 10 years earlier in the light-skinned French women than in their Chinese peers. This is consistent with the observation that fair-skinned Western Europeans are more likely to develop wrinkles than other ethnicities (45). But, systematic studies on this topic are scarce (41).
The research team around Abigail Langton is dedicated to the systematic study of the skin aging in dark-skinned people. (46-48).
But also for ethnic skin the well-known effects of solar elastosis - the degradation of elastin by UV light - can be observed. So is the extrinsic flattening of the interlocking of epidermis and dermis. There are no data yet on possible differences in repair and regeneration mechanisms depending on genetics. However, initial orienting studies on the relevant elastic components of the ECM suggest that these are also genetically determined (49). Also known are the differences in the collagen structure of different ethnic groups (13). To what extent these genetic factors influence the aging process of the skin is not yet fully understood.
Therapy of skin aging or prophylaxis?
The list of active ingredients for anti-aging purposes is long. The market is large and yet, the efficacy is limited. Even though collagen drinks (50) and anti-wrinkle creams are booming, they in reality only treat the symptoms. Since the relevant events of skin aging take place in the dermis, one can assume, that cosmetic ingredients are not able to reach this part through the epidermis. In other words, anti-aging ingredients only have a superficial effect. Even if the manufacturers want to persuade us to buy these products and promise great effects and proven efficacy in in vitro tests. A relevant wrinkle correction can only be achieved with more "drastic" methods, such as chemical peeling, plasma treatments, needling or a surgical intervention.
Nevertheless, in the complex process of skin aging, there is not one factor that can be "corrected" alone.
However, the studies of many researchers prove that we can control skin aging rather with our personal lifestyle than with cosmetics. In short, with prophylaxis. But, this does not mean using anti-wrinkle products as a teenager, as some might think, but avoiding certain risks.
The main factors that cause premature aging of the skin are UV radiation and smoking. However, simple things such as a balanced diet, which Millar (51) summarizes in her 2018 article, are helpful.
References
(1) Martvolumen von Anti-Aging Produkten
(2) Lemperle G. et al. A classification of facial wrinkles (2015)
(3) Gunn DA. et. al. Why some women look young for their age PLOS one (2009)
(4) Dobos, G., Lichterfeld, A., Blume-Peytavi, U. and Kottner, J. (2015), Evaluation of skin ageing: a systematic review of clinical scales. Br J Dermatol, 172: 1249-1261
(5) Addor FAS. Beyond photoaging: additional factors involved in the process of skin aging. Clin Cosmet Investig Dermatol. 2018 Sep 20;11:437-443. doi: 10.2147/CCID.S177448. PMID: 30288075; PMCID: PMC6159789.
(6) Pawlaczyk M, Lelonkiewicz M, Wieczorowski M. Age-dependent biomechanical properties of the skin. Postepy Dermatol Alergol. 2013 Oct;30(5):302-6. doi: 10.5114/pdia.2013.38359. Epub 2013 Oct 30. PMID: 24353490; PMCID: PMC3858658.
(7) DejaYu: Stratum Corneum und der washout-Effekt
(8) Walek J. Bindegewebe, Bibliothek der Anatomie (2022)
(9) Ziemer M., Histopathologie der Haut – Bindegewebekrankheiten, Springer Medizin
(10) Pfisterer K. et.al.The Extracellular Matrix in Skin Inflammation and Infection, Frontiers in Cell and Developmental Biology (2021)
(11) Naylor EC, Watson RE, Sherratt MJ. Molecular aspects of skin ageing. Maturitas. 2011 Jul;69(3):249-56. (12) Bielajew, B.J., Hu, J.C. & Athanasiou, K.A. Collagen: quantification, biomechanics and role of minor subtypes in cartilage. Nat Rev Mater 5, 730–747 (2020)
(13) Chan T-F. et. al, Natural variation in four human collagen genes across an ethnically diverse population, Genomics (2008) Vol 91 (4), 307-314
(14) Scarr G., Simple geometry in complex organisms, Journal of Bodywork and Movement Therapies (201), Vol 14(4), 424-444
(15) Wikipedia Commons: Tendon-anatomy
(16) Wikipedia: Kollagen
(17) Haq F, Ahmed N, Qasim M. Comparative genomic analysis of collagen gene diversity. 3 Biotech. 2019;9(3):83
(18) Wikipedia.org:Collagen
(19) Baumann L, Bernstein EF, Weiss AS, et al. Clinical Relevance of Elastin in the Structure and Function of Skin. Aesthet Surg J Open Forum. 2021;3(3)
(20) Kristensen JH, Karsdal MA, Chapter 30 – Elastin, Biochemistry of Collagens, Laminins and Elastin, Academic Press (2016) 197-201
(21) Van Doren SR. Matrix metalloproteinase interactions with collagen and elastin. Matrix Biol. 2015;44-46:224-231.
(22) Freitas-Rodríguez S. et al., The role of matrix metalloproteinases in aging: Tissue remodeling and beyond, Biochimica et Biophysica Acta (BBA) – Molecular Cell Research (2017),Vol. 1864, 2015-2025
(23) Sawakinome: Unterschied Kollagen und Elastin
(24) Kruglikov IL, Scherer PE. Skin aging as a mechanical phenomenon: The main weak links. Nutr Healthy Aging. 2018;4(4):291-307.
(25) Tracy LE, Minasian RA, Caterson EJ. Extracellular Matrix and Dermal Fibroblast Function in the Healing Wound. Adv Wound Care (New Rochelle). 2016;5(3):119-136.
(26) Wikipedia.org: Fibroblast
(27) Schuster, R, Rockel, JS, Kapoor, M, Hinz, B. The inflammatory speech of fibroblasts. Immunol Rev. 2021; 302: 126– 146
(28) Dellambra E, Dimri GP, Chapter 7 – Cellular Senescence and Skin Aging, In Personal Care & Cosmetic Technology, Skin Aging Handbook, William Andrew Publishing (2009), 129-148.
(29) Cole MA, Quan T, Voorhees JJ, Fisher GJ. Extracellular matrix regulation of fibroblast function: redefining our perspective on skin aging. J Cell Commun Signal. 2018;12(1):35-43.
(30) Mine S, Fortunel NO, Pageon H, Asselineau D (2008) Aging Alters Functionally Human Dermal Papillary Fibroblasts but Not Reticular Fibroblasts: A New View of Skin Morphogenesis and Aging. PLoS ONE 3(12): e4066.
(31) Lee DH, Oh JH, Chung JH. Glycosaminoglycan and proteoglycan in skin aging. J Dermatol Sci. 2016 Sep;83(3):174-81.
(32) Lauren E. Tracy, Raquel A. Minasian, and E.J. Caterson.Advances in Wound Care.Mar 2016.119-136.
(33) Dermaviduals: Hyaluronsäure
(34) Papakonstantinou E, Roth M, Karakiulakis G. Hyaluronic acid: A key molecule in skin aging. Dermatoendocrinol. 2012;4(3):253-258.
(35) Bruckner-Tuderman L, Has C, Disorders of the cutaneous basement membrane zone—The paradigm of epidermolysis bullosa, Matrix Biology (2014), Vol. 33, 29-34.
(36) Schmidt E, Zilikens D, Pemphigoid diseases, The Lancet (2013), Vol.381 ( 9863), 320-332.
(37) Yang, S., Sun, Y., Geng, Z., Ma, K., Sun, X., Fu, X.”Abnormalities in the basement membrane structure promote basal keratinocytes in the epidermis of hypertrophic scars to adopt a proliferative phenotype”. International Journal of Molecular Medicine 37, no. 5 (2016): 1263-1273.
(38) Langton AK et. al. , The impact of intrinsic ageing on the protein composition of the dermal-epidermal junction, Mechanisms of Ageing and Development (2016), Vol. 156, 14-16.
(39) Roig-Rosello E, Rousselle P. The Human Epidermal Basement Membrane: A Shaped and Cell Instructive Platform That Aging Slowly Alters. Biomolecules. 2020; 10(12):1607.
(40) Feru J, Delobbe E, Ramont L, Brassart B, Terryn C, Dupont-Deshorgue A, Garbar C, Monboisse JC, Maquart FX, Brassart-Pasco S. Aging decreases collagen IV expression in vivo in the dermo-epidermal junction and in vitro in dermal fibroblasts: possible involvement of TGF-β1. Eur J Dermatol. 2016 Aug 1;26(4):350-60.
(41) Vashi NA, de Castro Maymone MB, Kundu RV. Aging Differences in Ethnic Skin. J Clin Aesthet Dermatol. 2016;9(1):31-38.
(42) BBC: Does darker skin wrinkles less?
(43) Makrantonaki E. et al., Genetics and skin aging, Dermato-Endocrinology (2012), 280-284.
(44) Nouveau-Richard S, Yang Z, Mac-Mary S, Li L, Bastien P, Tardy I, Bouillon C, Humbert P, de Lacharrière O. Skin ageing: a comparison between Chinese and European populations. A pilot study. J Dermatol Sci. 2005 Dec;40(3):187-93.
(45) Peptan:Does ethnicity affect how skin ages?
(46) Langton AK et al. Aging in Skin of Color: Disruption to Elastic Fiber Organization Is Detrimental to Skin’s Biomechanical Function, Journal of Investigative Dermatology (2019), Vol. 113 (4), 779-788.
(47) Langton, A., Graham, H., McConnell, J., Sherratt, M., Griffiths, C. and Watson, R. (2017), Organization of the dermal matrix impacts the biomechanical properties of skin. Br J Dermatol, 177: 818-827.
(48) Langton AK, Alessi S, Hann M, Chien AL, Kang S, Griffiths CEM, Watson REB. Aging in Skin of Color: Disruption to Elastic Fiber Organization Is Detrimental to Skin’s Biomechanical Function. J Invest Dermatol. 2019 Apr;139(4):779-788.
(49) Langton, AK, Hann, M, Costello, P, et al. Heterogeneity of fibrillin-rich microfibrils extracted from human skin of diverse ethnicity. J Anat. 2020; 237: 478– 486.
(50) Pinkmelon: Trinkkollagen
(51) Millar SE, Revitalizing Aging Skin through Diet, Cell (2018), Vol. 175 (6) 1461-1463.
Picture credits
All tables, own work and can be uses under the Creative Commons licence CC BY-SA 3.0
Figures 1 and 3, own work and can be uses under the Creative Commons licence CC BY-SA 3.0
Figure 2: https://pubmed.ncbi.nlm.nih.gov/21612880/
Figure 4: https://www.mdpi.com/2218-273X/10/12/1607/htm
Figure 5: https://pubmed.ncbi.nlm.nih.gov/30404021/












