By: René Serbon
Chair of the Education Board, The International Association for Applied Corneotherapy
CEO, Dermal Systems Inc.
In layman's terms, healthy skin is described to clients as a balance of water and oil in the skin. Too much or too little of one or the other can lead to an impaired skin barrier, and excess of one or the other can fuel skin conditions and disorders; for example, excess water can fuel rosacea sub-type 2.
Society typically understands what we mean when we say oily skin and even knows its visual appearance. However, what are the clinical symptoms of water imbalance in the skin? Unfortunately, compromised skin often does not show apparent indicators, and the indicators or symptoms can be subtle but could lead to troublesome skin conditions.
A water imbalance leads to an electrolyte imbalance. Electrolytes are so-called because they have an electrical charge and include, for example, salt, potassium, calcium, and chloride. Electrolytes are mentioned because they are essential and bodily processes require a small electrical current which triggers an interaction with each other and our nerves, tissues, and muscles. Different electrolytes carry out different processes in our bodies and the skin, such as regulating bodily hydration, controlling blood pressure, and helping repair damaged tissue. [Fig 1.]
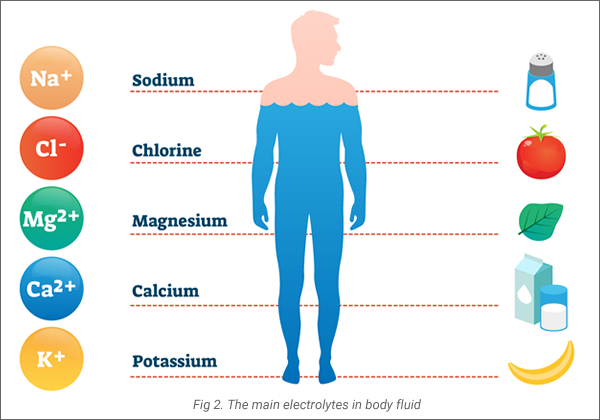
Ultimately it plays a vital role in functions that keep us alive. The development of our brain and nerves. Growth of our muscles. The creation of new tissue. These are all dependent on electrolyte activity within our bodies. [Fig 2]
Our bodies show electrolyte imbalance via common symptoms that can include dizziness, fatigue, and muscle spasms to severe symptoms such as seizures and even comas. So what would water and electrolyte imbalance mean for our skin if the body could respond this way to electrolyte imbalance? 75 to 80 percent of our body is comprised of water at birth. This percentage dwindles to about 60 percent for men and 55 percent for women by adulthood and continues to decrease as we age. Water and electrolytes are essential to health.
To put the importance of water into perspective related to electrolytes, remember that electrolytes are minerals that conduct electricity when mixed with water. It is similar to switching on a light, where once turned on, it sparks a chain reaction triggering the cells to 'do its work.'
These electrolyte minerals dissolve in the body's fluids, including the skin, support a healthy fluid balance, and facilitate the transfer of nutrients into cells while simultaneously removing waste. Our skin gets supplied with electrolytes via blood vessels from the food we eat and the water we drink.
As practicing corneotherapists with a deep understanding of the keratinocyte lifecycle, there are critical cellular activities that we aim to optimize in order to support strong skin barrier function. Considering the importance of water balance in the skin, one must understand what cellular activities require water for the skin to function.
Skin is our largest organ, and the epidermis (particularly the stratum corneum) provides a barrier against environmental influences such as allergens, pathogens, and pollutants. The epidermis also protects against excessive water loss.
The keratinocyte lifecycle is a process of terminal differentiation. Keratinocytes proliferate starting at the basal layer of the epidermis to continuously self-renew. Once they start their terminal journey upward, they start to differentiate in a sequence of events until they finally reach the skin's surface as a corneocyte and desquamate.
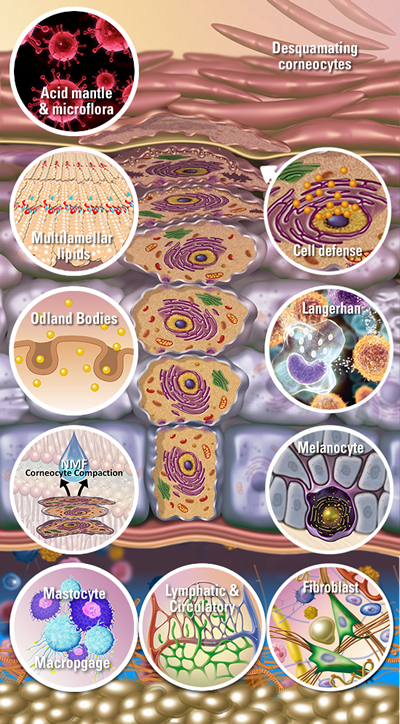
In the stratum granulosum, during this upward migration of the cells to the skin surface, the keratinocyte undergoes several changes in its structure and composition. These changes contribute to the skin barrier defense systems by forming the lamellar lipid structure, cornifying the cell envelope, dissolution of the desmosomes, and forming the hydrating Natural Moisturizing Factor (NMF), along with corneocyte compaction and nucleus deactivation.
The keratin fibrils are becoming more structured. The cell shape is changing, beginning to flatten. The critical formation of the corneocyte's chemically, and physically resistant cornified cell envelope begins. Once the cell's nucleus deactivates, it completes the release of Odland bodies and NMF (more on this later) and becomes a corneocyte. In the stratum corneum, corneocytes are ingrained in the intercellular lipid matrix.
During this process, intracellular Ca2+ levels rise, the transglutaminase 1 enzyme is expressed, and it spontaneously assembles onto membranes joining the plakins and involucrin together by forming crosslinks. Additionally, it crosslinks other membrane-associated and desmosomal proteins, changing the dynamic properties of cell junctions and cytoskeletal interactions. Gradually, the proteins form a monomolecular layer along the entire inner surface of the plasma membrane, including over desmosomes, to form a scaffold for the deposition of the extracellular lamellar lipid structure.
The cornified envelope not only protects against external injury but also serves as a scaffold for the deposition of the extracellular lamellar bilayers. These organize extracellular lipids into orderly lamellae. Together, the cell envelope and extracellular lipids are essential for effective physical and water barrier function in the skin.
Almost parallel to the cornification of the cell envelope, the formation of the Odland bodies takes place and plays a vital role in the preparation of the desquamation process. More about this process involving enzymes can be read in this Journal in Florence Barrett-Hills' article ‘Water-enzymes and lipid metabolism.
For this discussion, I want to summarize in short that once, the lamellar bodies (from the Odland bodies) are ejected by the method of exocytosis at the interface between the stratum corneum and stratum granulosum, a densely packed intercellular lipid matrix is formed from the metabolized lipids. This action is essential for many reasons. However, the key concerning water imbalance in the skin is that this lipid matrix helps retain water in the skin, and it plays a role in the dissolution of the corneodesmosomes to facilitate desquamation ultimately.
A core process of desquamation is the degradation of corneodesmosomes. Corneodesmasomes are the proteins that bind the intercellular regions. They degrade toward the surface of the stratum corneum in order to shed surface corneocytes.
Enzyme activity is again the regulator for the degradation of corneodesmosomes. Some enzymes involved are most active in an acidic environment, whereas others are optimal in a pH-neutral environment. In either case, enzyme activity is dependent on water in the enzyme's microenvironment, noting that the closer the cells get to the skin's surface, the lower the water content in the skin.
Hygroscopic molecules in corneocytes retain sufficient amounts of water in the stratum corneum. Filaggrin is a well-known source of these natural moisturizing factors. In addition, water is necessary for the procreation of NMF itself.
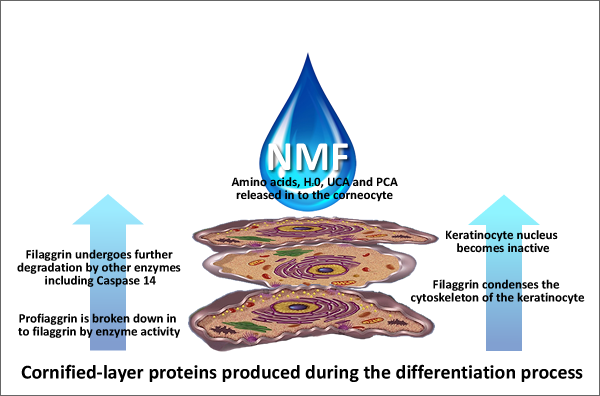
The procreation of NMF is a phase that takes place in synergy with the formation of the cornifies cell envelope and the lipids formation of the Odland body and takes place in the upper granular layer. The production of amino acids begins with a protein called profilaggrin which is stored in the keratohyalin granules. In response to calcium levels and enzymes such as caspase 14, the keratohyalin granules de-granulate. Profilaggrin gets broken down into filaggrin and then into free amino acids and derivatives such as urocanic acid and pyrrolidone carboxylic acid. These are collectively referred to as natural moisturizing factors (NMF), a major contributor to skin cell hydration.
In the stratum corneum, the released filaggrin monomers bind keratin filaments, instigating their collapse into thickened and aggregated keratin filaments, which condenses the keratinocyte cytoskeleton. Simultaneously at this point, the nucleus of the keratinocyte is rendered inactivated.
As corneotherapists, we can conclude that a water imbalance in the skin will result in a compromised skin barrier at its basis. As mentioned, these symptoms might not always be evident, and early detection of diagnostic clues is paramount for early intervention to prevent certain conditions from becoming disorders.
Some of the diagnostic clues that will result include:
● Cracked and dry lips
● Itchy skin
● Inflammation
● Dullness
● Darker under-eye circles
● Sunken eyes
● Increase of and fine lines surface wrinkles (especially in a short timeframe)
● Low readings on diagnostic equipment
When left untreated and unaddressed, it can compound into or contribute to conditions and disorders such as:
● Flaking dry patches
● Psoriasis
● Dermatitis/Eczema
● Rosacea
● Ichthyosis
● Xerosis
● Corneocyte compaction disorders
Water has always been essential to sustaining life, and educating clients on the importance of a healthy water balance is empowering to help them monitor their skin health. In addition, with better knowledge, understanding when to consume more or less water helps empower clients into better compliance. Finally, it gives them the tools to adjust adequately to their environment (high or low humidity) and lifestyle choices (exercise, work, play).
About the author:
René Serbon is CIDESCO, and CIBTAC certified, one of the world’s few Pastiche Accredited Educators and proudly serves on the International Association of Applied Corneotherapy (IAC) educational board. – A practising corneotherapist, industry educator and speaker - gives skin care professionals a genuine point of difference in the industry. How? By handing them the ultimate drawing card: knowledge about the skin wrapped in savvy business strategy.
Her keynotes and in-depth training educate on skin anatomy, physiology, and how to match cosmetic chemistry to specific skin conditions - helping clinic owners and solo estheticians increase their in-clinic results and business growth (by 30% a year or more).
ARTICLE REFERENCES:
Journal of Investigative Dermatology, Volume 128, Issue 2, February 2008, Pages 378-388, Water Distribution and Natural Moisturizer Factor Content in Human Skin Equivalents Are Regulated by Environmental Relative Humidity ( https://reader.elsevier.com/reader/sd/pii/S0022202X15337441?token=0530FD4E5EE2435C96A51DB70707852EB1F4DFCA5BBEDD546B9C74B1C0014DE7151092F19388539F85B42E157C03B67A&originRegion=us-east-1&originCreation=20220713185509 )
https://dermaviduals.de/english/publications/problem-skin/enzymes-to-inhibit-or-to-stimulate.html
https://www.healthgrades.com/right-care/symptoms-and-conditions/electrolyte-imbalance
https://medlineplus.gov/ency/article/001187.htm
https://www.medicalnewstoday.com/articles/electrolyte-imbalance
Advanced Skin Analysis, Florence Barrett-Hill ISBN 978-0-473-25052-2
Cosmetic Chemistry, Florence Barrett-Hill ISBN 978-0-473-26279-2













